Create your free resume and start your job search today.
Try it out - it's Free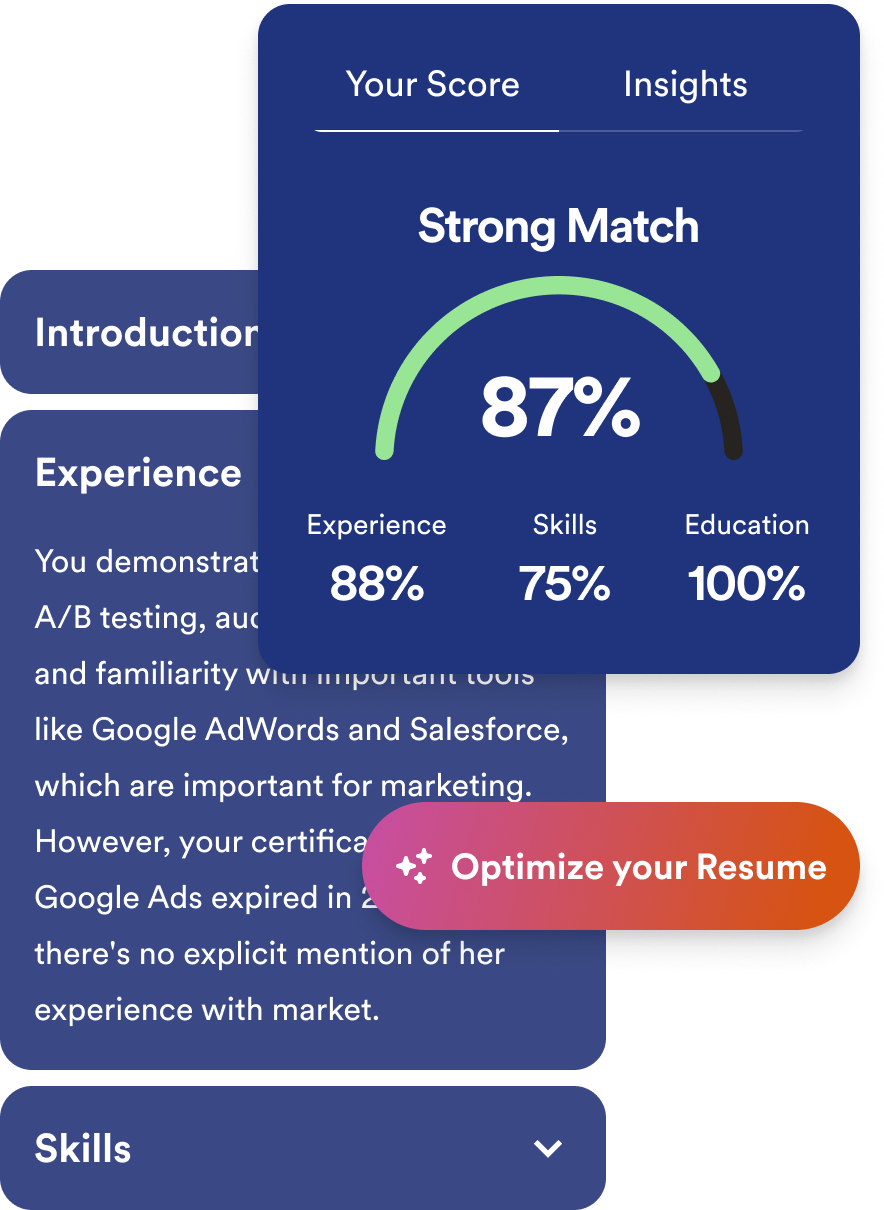

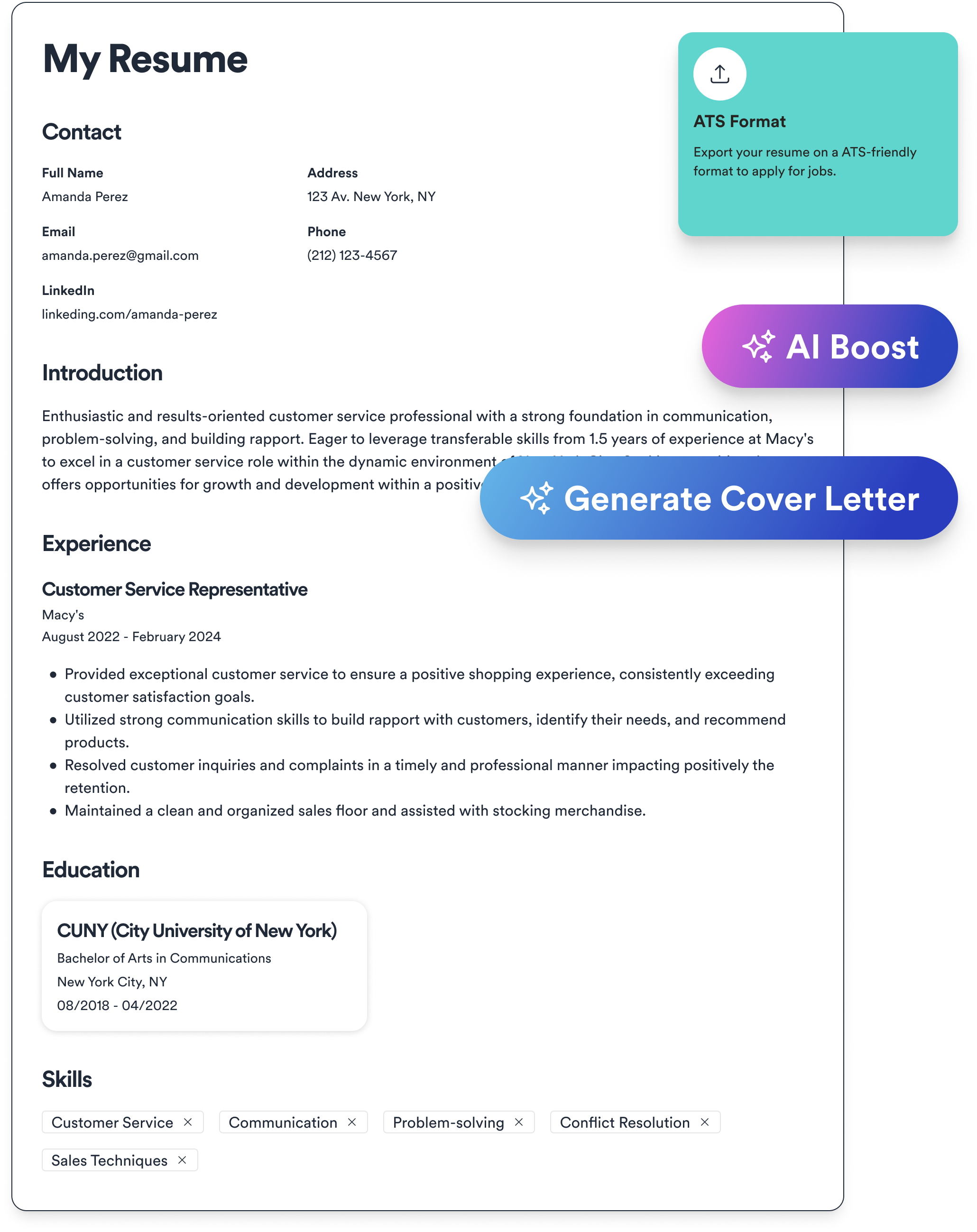
Transform your work experience into an ATS-friendly resume that hiring managers can't ignore. Our free resume builder helps you craft a professionally formatted resume that highlights your most relevant skills and experiences, saving you time while maximizing your chances of getting past automated screening systems.
See exactly how well your resume matches each job opportunity. Our intelligent scoring system analyzes your resume against specific job descriptions, providing actionable feedback to help improve your match rate and identify skill gaps that could be holding you back.

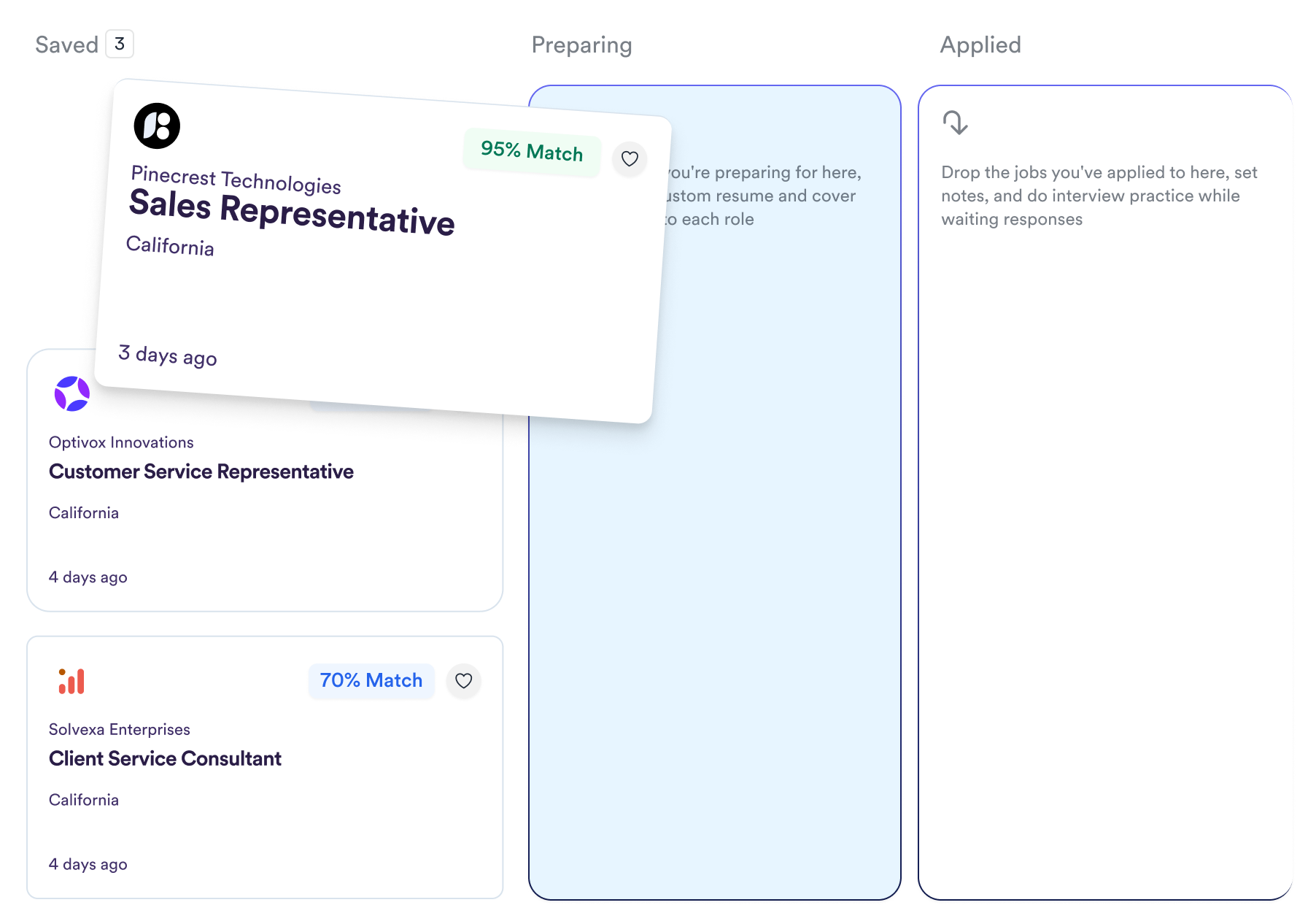
Avoid losing track of your job applications. Our comprehensive job application tracker helps organize your career search journey - from saved positions to applications in progress and scheduled interviews. Keep everything in one place and make informed decisions about where to invest your energy.
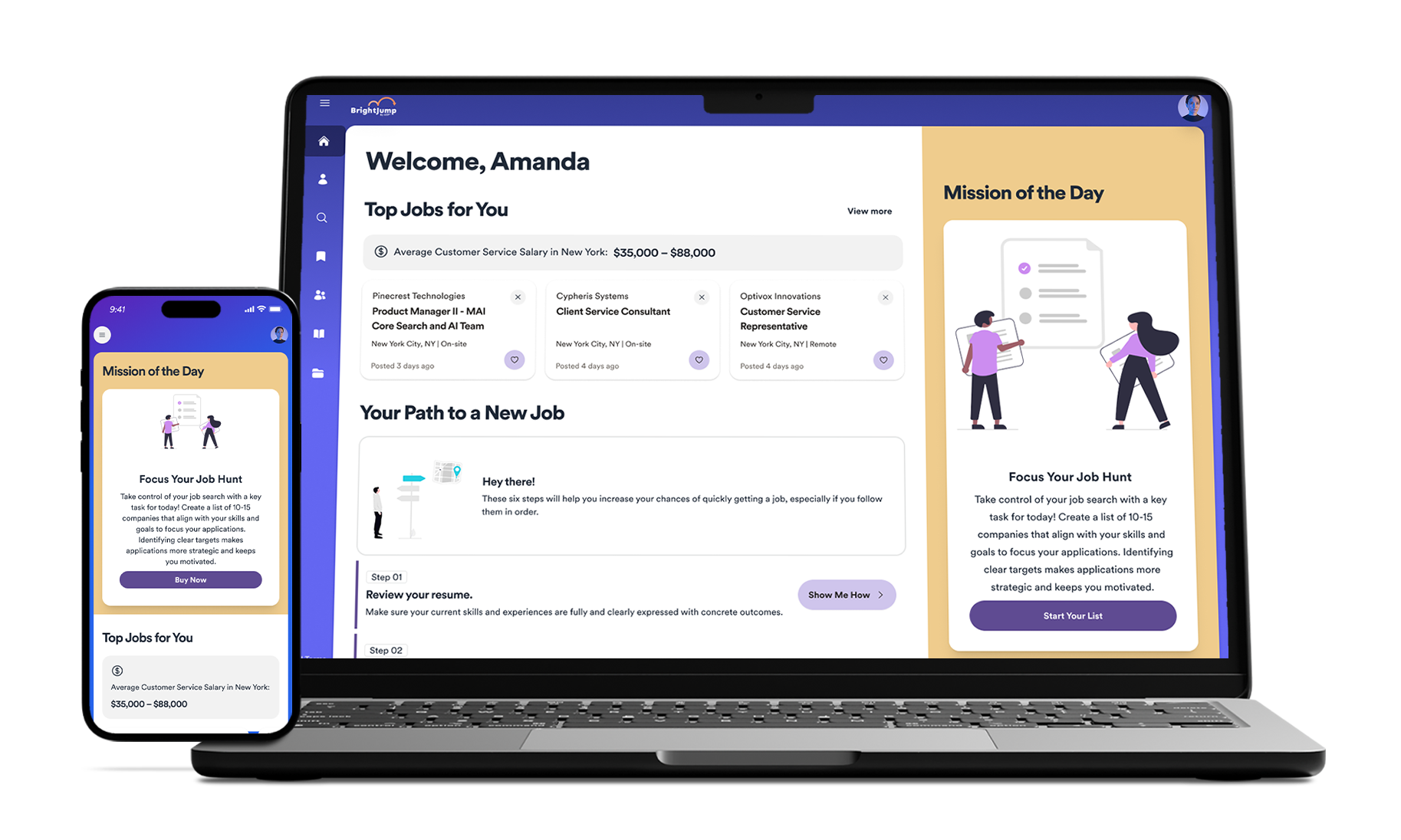
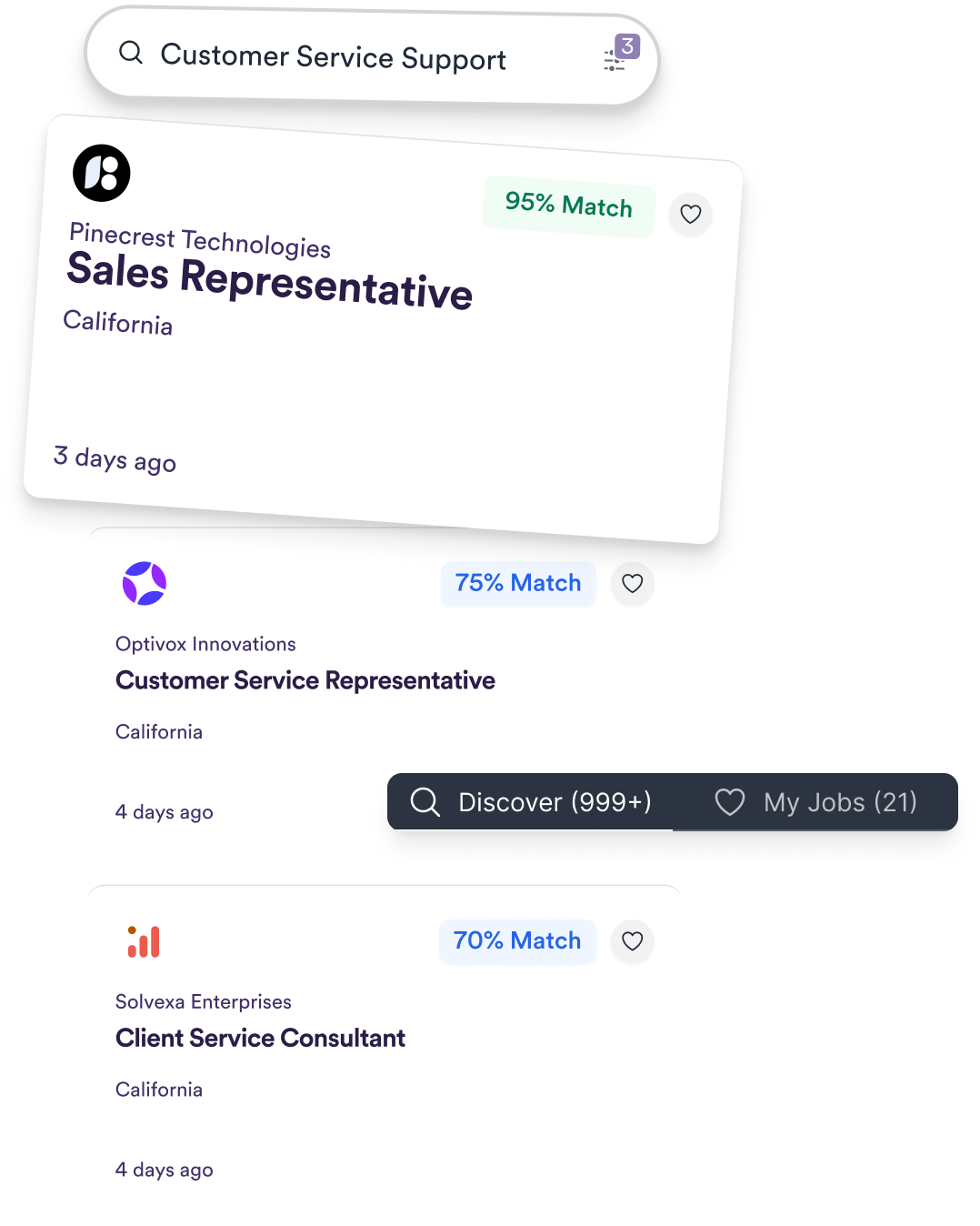
Access over 3.2 million verified US job listings with accurate posting dates and active status indicators. Our job board helps eliminate fake listings and connects you directly to employer sites with just one click, helping you discover opportunities that perfectly align with your career goals.
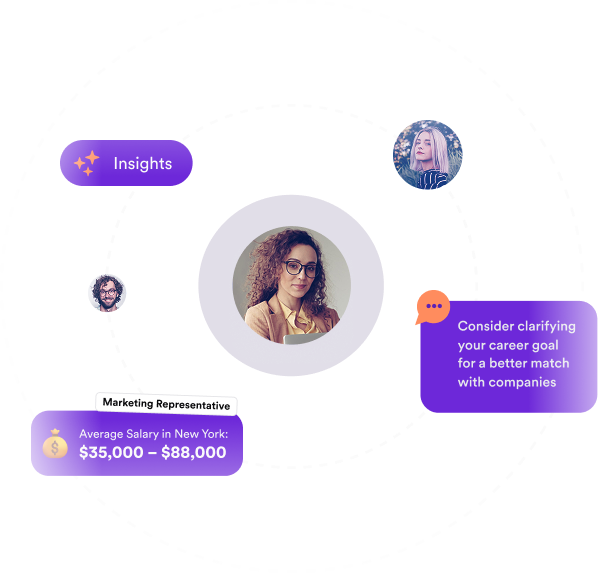
Get noticed by top recruiters searching for talent like you. Gain visibility with thousands of hiring professionals who can view your profile and request interviews. Update your visibility preferences anytime - whether you're actively job-seeking or prefer to stay private until the right opportunity comes along.
Take advantage of BrightJump’s free tools, tips, and support.
Create A Free Account Now